Published On September 22, 2005
“PERIODICITY IS DEAD,” proclaims Edwin Kilbourne, and he ought to know. Kilbourne is a physician who has witnessed the devastating toll pandemic flu can take on the elderly, pregnant women and people with heart disease. He cared for them at New York Hospital in Manhattan during the Asian flu outbreak that began in Yunan, China, in the spring of 1957 and soon swept the world. And he watched them die of a viral pneumonia quite like the one that killed millions during the deadly influenza outbreak of 1918.
Eleven years later, the Hong Kong flu pandemic hit, taking the lives of an estimated 34,000 people in the U.S. alone. Kilbourne and other flu experts became convinced that such outbreaks were periodic, emerging every 10 years or so. They based this notion solely on the perception that outbreaks seemed to occur fairly regularly, though how, and through what mechanism, was never explained. Then in 1976, when a young soldier at Fort Dix, N.J., died of a virus suspiciously like the 1918 flu bug, Kilbourne and others argued that another deadly pandemic was imminent. The U.S. government rushed a vaccine into production and inoculated 40 million people. About 25 died of vaccine-related complications, but the swine flu outbreak never materialized, and no pandemic strain has emerged since.
Despite that long quiescence—or because of it—flu specialists at the U.S. Centers for Disease Control and Prevention (CDC) and at the World Health Organization (WHO) consider a deadly global outbreak long overdue. They’re anxiously watching a new virus known as H5N1, which has ravaged Asian poultry flocks and by early last summer had killed more than 50 people. Tim Uyeki, a leading epidemiologist at the CDC, has warned of a looming public health disaster, as have several WHO officials. Recent articles in Nature, Foreign Affairs and The New England Journal of Medicine have suggested that a lethal pandemic is in the offing—and that we, as a nation and as a species, are not prepared for the eruption of what could be the deadliest plague of all.
Kilbourne, currently emeritus professor of microbiology and immunology at New York Medical College, chides those at the WHO and the CDC who insist that we’re overdue for a pandemic. As for the very notion of periodicity, Kilbourne says: “Periodicity has really fallen apart as a concept because of what’s happened since 1968. We have had no pandemics in the twenty-first century. We have H3N2—Hong Kong flu—circulating still. No strain has yet replaced it. The CDC and WHO shouldn’t be talking about periodicity.”
That is not to say, of course, that a pandemic could not emerge. Each year, a new strain of influenza spreads across the globe, sickening millions; according to the CDC, in a typical year an estimated 36,000 Americans die from influenza-related complications and more than 200,000 are hospitalized. But when flu experts speak of a coming pandemic, they’re describing something potentially far more devastating. The concern is that, rather than a slight genetic variation on last year’s virus, a wholly new form could develop and spread wildly, cutting down millions who have no natural resistance.

VITO PALMISANO/GETTY IMAGES
THE EVENT THAT COULD TRIGGER A PANDEMIC is a switch in the proteins—hemagglutinin (HA) and neuraminidase (NA)—that project from the surface of the flu virus. Within each of these antigen types lies considerable variation. If a population is already largely immune to a particular variant, natural selection will favor the spread of mutations in the genes for HA or NA. Known as antigenic drift, these small changes in the structure of the proteins result in a variant of the existing virus that is just different enough from the last version to stay one step ahead of the body’s immune system. Then, as immunity catches up, the virus evolves again.
Occasionally, though, an entirely new class of surface antigen replaces the currently circulating HA protein through reassortment with genes of another species, usually birds—an occurrence known as antigenic shift. Sixteen types of HA have been recognized in wild bird populations, and six or so are believed capable of producing human disease. When the new antigen replaces the existing HA protein—as when H1 yielded to H2 in 1957—people have no resistance to the new HA, and a pandemic ensues. H1, H2 and H3 were responsible, respectively, for the past three pandemics. Now it’s the H5N1 virus that is stirring fears of an imminent deadly outbreak.
DURING THE PAST DECADE, H5N1 has evolved as a vicious chicken killer. A form of the virus first emerged among geese in China’s southern Guangdong Province in 1996, and by 1997 several people had also died. Rapid intervention eliminated that particular variant. (Millions of chickens were culled, and Asia’s “wet markets”—where thousands of live chickens, ducks, geese, other poultry and other animals are crammed into small cages to await selection and slaughter—were thoroughly hosed down and scrubbed with disinfectant.) But a descendant of the lethal H5 protein continued to circulate, and by 2003, another chicken-killing H5N1, with an H5 gene similar to 1997’s, burned through the farms and markets of Asia. This strain, which flu researchers call the Z form of H5N1, is now prevalent from Thailand to Qinghai Province in western China.
H5, including the Z form, is deadly because it enables amino acids to accumulate at a particular site on the surface spikes of the HA protein—the site that must be cleaved, or split, to allow the virus particle to penetrate the host’s cell. These amino acids, in turn, allow the virus to infect many types of cells instead of just the respiratory or gastrointestinal cells that normal flu strains attack. That’s why H5 avian flu, in chickens, is a systemic disease.
Where did this lethal protein originate? All avian flu genes come from wild birds, according to avian influenza expert David Swayne, director of the Southeast Poultry Research Laboratory of the U.S. Department of Agriculture. H5N1 was probably a benign virus colonizing the intestines of wild waterfowl. Flying into farm ponds, they shed the virus in their feces, infecting domestic ducks. On Asian family farms, where ducks and chickens live together, the ducks infected the chickens, which were taken to market crammed together in wire baskets, providing an opportunity for the virus to spread as the birds passed it on through feces and the respiratory tract.
The ideal conditions for viral evolution, however, aren’t found on the way to market but on China’s and Thailand’s large-scale commercial farms, where several million chickens may be packed in close quarters. According to infectious disease expert Paul W. Ewald of the University of Louisville, the best way to “heat up” the virulence of a virus is to place its hosts in close proximity to other potential hosts. If a host must be mobile in order for a virus to spread, the disease cannot become extremely virulent. For example, the human influenza virus has to keep its hosts well enough to walk around, shake hands and sneeze in other people’s faces. But if people—or chickens—are crammed together, so that a host immobilized by illness can still transmit the disease to another host, the brakes are off. The disease grows hotter and hotter as the viral strains best adapted to exploit the host’s tissues race through the victim, overcoming milder strains while avoiding any penalty for killing the host because another is close at hand.
Biosecurity at large-scale farms in Thailand, Vietnam and other affected areas has improved, says Swayne. Birds must now be certified free of infection before they’re sold or moved, and they’re kept in supposedly cleaner, less crowded conditions. But small family farms, ubiquitous in Southeast Asia, continue to be breeding grounds for H5N1. Chickens, ducks and geese, free to run about the farmyard, shed infected feces onto the ground or into water, and lethal flu is transported by the movements of both live poultry and meat, which poses a threat during food preparation or if meat scraps are fed to other birds. Even feces on the boots of farmers have helped carry deadly strains of the virus across Asia.

THE ART ARCHIVE/IMPERIAL WAR MUSEUM
There is another possible culprit—migratory birds—although their role is debated. Late last spring, 1,000 dead fowl of five different species were found near Qinghai Lake, a bird reserve in western China, and another 500 dead birds were discovered in the neighboring far western Xinjiang Province near Mongolia. The Chinese government contends that these birds brought the flu virus with them, and that otherwise H5N1 did not exist in China. But that’s a claim many flu researchers dismiss.
“Dead ducks don’t fly,” says Alan P. Zelicoff, a disease surveillance expert at Ares Corp., a provider of risk- and project-management services to government agencies in Albuquerque. Though some wild birds may be able to travel short distances immediately after being infected, it’s hard to believe they could survive a flight across the Himalayas—on their way from the lowland marshes of northern India to their breeding grounds in the high plateaus of Central Asia—carrying an infection as lethal as this one. So it’s quite likely that both wild and domestic birds in China are widely infected, and that they’re spreading the disease to migratory birds through feces.
Besides, if Ewald is correct, the virus in flu-infected wild birds should become less, not more, virulent. For the disease to sustain itself among wildfowl, the birds must remain well enough to carry it along their migratory paths. And according to Richard Webby, a flu researcher at St. Jude Children’s Research Hospital in Memphis, that is exactly what’s happening. Strains of the H5N1 virus taken from Asian ducks seem to be evolving back toward benignity.
WHEN H5N1 JUMPS FROM BIRDS TO PEOPLE—normally through contact with feces or during the preparation of raw chicken or duck meat—it may be quite virulent. The death rate among those known to have been infected has averaged around 70%—compared with a maximum of 5% now calculated for the 1918 flu, which may have killed as many as 50 million people. Some scientists have suggested that all that is necessary for an outbreak worse than that of 1918 is for the disease to evolve into a form easily transmitted from human to human.
In theory, H5N1 could produce a new pandemic in two ways. First, the avian virus could reassort with common, highly transmissible human flu strains. H5N1 binds preferentially to avian receptor cells in the respiratory tract—and humans also have some cells with avianlike receptors. For reassortment to take place, a human flu strain and an avian one must infect the same cell at the same time—meaning that the host must contract both infections within a short period. As unlikely as this may seem, molecular tests reveal that is precisely what happened to create the pandemic flu strains of 1957 and 1968.
Without reassortment, H5N1 could conceivably evolve enhanced transmissibility simply by cycling from person to person. But for that to occur, the virus would have to develop the ability to colonize the upper respiratory tract, where particles can be readily coughed or sneezed out. According to Earl Brown, molecular virologist and flu researcher at the University of Ottawa, the latest autopsy reports on a patient who died of H5N1 infection after a 17-day hospitalization show virus particles only deep in lung tissue, not high up in the windpipe or nasal passages. This may explain why H5N1 isn’t readily transmitted—and why, unlike severe acute respiratory syndrome (SARS), even hospital workers don’t seem to catch it.
Even if a more transmissible virus evolves, its virulence would likely decline sharply. The only flu pandemic lethal to healthy people was incubated in the trenches, trucks, trains and hospitals of World War I’s Western Front. As Ewald has suggested and as historian of military medicine Carol R. Byerly demonstrates in her recent book, Fever of War, these conditions allowed terrifying flu strains to develop among the immobilized sick and wounded, just as avian flu has gained strength in the packed chicken farms of Asia. Then, when the war ended, the disease lost its virulence, becoming nothing more than the common flu.
Kilbourne, veteran of two pandemics and a frequent consultant to the government on the flu, cites another reason why H5N1 is unlikely to become a lethal human threat. The NA component of H5N1—the N1 class of proteins—is hardly novel to the modern world. The 1918 flu itself had an N1 component, and after it lost its virulence, H1N1 circulated the globe until the pandemic of 1957, when it was replaced by H2N2, which in turn was supplanted in 1968 by H3N2. Yet, while some 70,000 people died of H2N2 in the U.S. during 1957 and 1958, H3N2 caused only about half as many deaths. Kilbourne thinks that’s because the N2 portion of H3N2 conferred some immunity in 1968.
Perhaps as the result of a laboratory or vaccination accident, H1N1, now known as the Russian flu, began circulating again in 1977, and much of the world’s population has since been exposed to a form of N1. That should have induced some level of protection against H5N1 as well, Kilbourne says. While HA is most responsible for infectivity, NA also plays a crucial role. Immunity to the NA proteins slows the release of virus particles from an infected cell and limits the spread of the virus within the body.
The age of human flu victims during the current outbreak and the severity of their symptoms APPEAR to support Kilbourne’s thesis that N1 exposure may be mitigating H5N1’s threat. With many infectious diseases, severity increases with age. Yet from the beginning of this outbreak, H5N1 has infected mostly children and young people—those least likely to have prior N1 immunity. Moreover, the death rate from H5N1 seems to be dropping as the age range broadens. In southern Vietnam, where the age of those known to be infected so far ranges from two to 40, the death rate is 83.3%. But in northern Vietnam, the virus now infects people from under a year old to over 80—and mortality has dropped to 34%. This suggests that when older people are infected, they are less likely to die of the virus, perhaps, as Kilbourne thinks, because they’ve had previous N1 exposure that conferred some protection against H5N1.
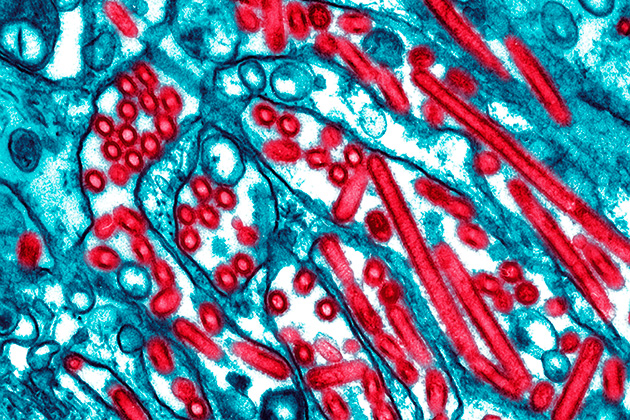
CDC/GOLDSMITH/KATZ/ZAKI/PHOTO RESEARCHERS
A NEW FLU PANDEMIC IS NEITHER overdue nor inevitable. Yet it would be wrong to take the threat of influenza lightly. It’s a leading cause of sickness and death, especially among the old, the very young and those with compromised immune systems. Increased surveillance of both avian and human diseases around the world is essential. So is improved biosecurity on poultry farms. Approximately 130 million poultry have been destroyed since 2004, at an incalculable cost to small farmers and the economies of the affected nations. The development of vaccines and antiviral drugs is also crucial, with new technologies aimed at producing vaccines more quickly and with broader immunity likely to save lives and prevent suffering.
But underlying all those measures is the necessity to understand the evolutionary processes that produce disease outbreaks. Only a firm grasp of the evolutionary biology of flu—and of infectious disease in general—can help predict which disease outbreaks are truly threatening and guide us toward a rational strategy for coping with them.
Dossier
“The Human-Animal Link,” by William B. Karesh and Robert A. Cook,Foreign Affairs, July/Aug. 2005. The most valuable of the pieces in the magazine’s special section on the threat of avian flu.
“Capturing a Killer Flu Virus,” by Jeffery K. Taubenberger, Ann H. Reid and Thomas G. Fanning, Scientific American, Jan. 2005.Informative introduction to the techniques that allowed retrieval of sequences for the 1918 flu.
Fever of War, by Carol R. Byerly (NYU Press, 2005). An excellent history of the 1918 pandemic; Byerly has a firm grasp of evolutionary theory and provides a moving description of the conditions leading to the pandemic.
Stay on the frontiers of medicine
Related Stories
- Avian Flu, One Year Later
After the panic, the author of our article on avian flu discusses developments in the story.
- Playing Chicken
New avian flu work has sparked debate among researchers and security experts.