Published On January 15, 2006
IN MANY WAYS, IT WAS AN UTTERLY COMMONPLACE ENCOUNTER. During 20 minutes with nurse practitioner Les Peters, Tom Townsend answered questions about his health and submitted to a few basic tests while Peters updated Townsend’s medical records.
But in several other respects, the encounter was extraordinary. For one thing, it took place in a converted Greyhound bus parked next to the 4-H building in Moscow, Idaho. The bus is a traveling branch of the Spokane Veterans Affairs Medical Center, where Townsend, a 75-year-old veteran of the Korean and Vietnam wars, has been treated for a variety of conditions. Crisscrossing the region, Peters and his crew offer follow-up visits to patients who might otherwise have to drive long distances on less-than-ideal roads.
Also notable—in fact, unusual in medical care as practiced in this country—is that Townsend’s records are on Peters’s laptop, linked via the Internet to the medical center’s database. During the exam, Peters updated the file and renewed several of Townsend’s prescriptions without touching pen to paper. Though Townsend can scarcely believe it, this isn’t how things get done in most of American medicine, where paper files remain the norm, prescriptions are still written by hand and then deciphered by pharmacists, and physicians don’t carry computers wherever they go. Fewer than one in five U.S. hospitals have the information-processing capabilities that Veterans Health Administration patients have come to take for granted.
With 157 hospitals, nearly 900 outpatient clinics, 5.2 million patients and a budget of $30 billion in the 2005 fiscal year, the VHA is really a big, sprawling HMO, comparable in scale to such industry giants as Kaiser Permanente. And during the past decade—virtually overnight, in government time—its reputation has morphed from one of the nation’s worst health-care providers into one of the best. Now it’s leading the medical world into the era of digitized medicine, where sophisticated databases and high-speed computers will, in theory, produce a quantum leap in the quality of care.
LIKE MANY PARTS OF THE FEDERAL GOVERNMENT, the VHA was born small and fragmented and gradually coalesced, gaining its current name and cabinet status in 1989. But the VHA’s operating model was stuck in the 1950s: top-down, assembly-line-like, impersonal. Many decisions that ought to have been judgment calls were etched in bureaucratic stone. For example, “federal law required admission to get a prosthetic device, which meant if you sprained your ankle and needed crutches, you had to be admitted to the hospital, because crutches were considered a prosthetic device,” recalls Kenneth W. Kizer, a physician who was Under Secretary for Health in the Department of Veterans Affairs and CEO of the VHA from 1994 to 1999. The result of this and other arbitrary rules was that a lot of beds were occupied, at taxpayers’ expense, by veterans who should have been home with their families.
Beyond racking up unnecessary costs, all those hospitalizations exposed patients to potentially deadly perils. Spreading infections, incorrectly prescribed or administered medications, botched operations—the horror stories were so common that some politicians wanted to reform the whole system. Alabama senator Richard Shelby argued in 1992 on the Senate floor, “Peace for veterans in our VA hospitals is a hotter and deeper hell than the hell of war.”
But democracy often requires crisis to produce consensus, and 1994 was one of those rare times in the life of a bureaucracy when radical change was possible. Kizer was able to sit down with a blank sheet of paper and start sketching. In 1998, he recruited Jonathan Perlin (now the VHA’s Under Secretary for Health) to oversee quality and performance, and James Bagian, a former astronaut, to direct the VA National Center for Patient Safety.
To learn what they were up against, Kizer and his colleagues put in place quality-of-care measurements that had been developed but not yet widely deployed in the private sector. Held up to those metrics, the VHA system proved just as dysfunctional as its reputation suggested. Only one patient in four was getting the right immunizations, heart attack patients weren’t receiving lifesaving beta blockers, staffers were touching patients without washing their hands, and surgeons were operating on the wrong patients—or the wrong body parts.
As a government agency, the VHA couldn’t use stock options to change the behavior of its staff, all of whom were federal employees. But it could pound home the relevant ideas at staff meetings and publicize who was falling short. “Not all doctors were enthusiastic,” says Kizer. “Sometimes they didn’t like the performance measures we were using, so we said, ‘If it’s not a good measure, pick a better one, but we’re going to measure your performance and insist on the things that we know equate with good outcomes.’”
This combination of measurement and accountability brought changes that were at once commonsensical and profound. Kizer and his staff closed underutilized hospitals and reassigned patients. Many wards once packed with rows of beds—all the better for airborne pathogens—were converted to semiprivate rooms. Administrators put alcohol-cleansing-agent dispensers in or outside each room, making hand washing easier. Health-care workers began asking patients for name, birth date and Social Security number before putting them under. Outpatient procedures nearly doubled, while inpatient procedures declined by a third.
It worked. Infections and surgical mistakes fell, and the number of patients getting the right immunizations rose from 27% in 1995 to 80% in 2000. “And it’s very homogeneous across the system,” adds Kizer. “There used to be big differences between rural and urban, inpatient and outpatient groups. But today about 80% of all the VHA’s subgroups are immunized for influenza. That is radically better than in the private sector.”
These behavioral shifts could just as easily have been made in the 1950s. But the true agent of change was only starting to emerge as the VHA began restructuring. For more than a decade, VHA clerks had been entering paper records into a vast electronic database. For a private hospital, whose patients can move to another provider whenever they want, converting records for a computerized system has an uncertain payoff. But the VHA’s captive audience made such a project essential. Recognizing its value, Kizer’s team sped development of the database and implemented it systemwide.
From their laptop keyboards, VHA doctors can now order lab tests and medications and enter progress notes. The system also offers basic decision support, flagging patient drug allergies and potential drug interactions. Today a doctor who prescribes Coumadin for a patient on Motrin will be informed that she’s risking intestinal bleeding.
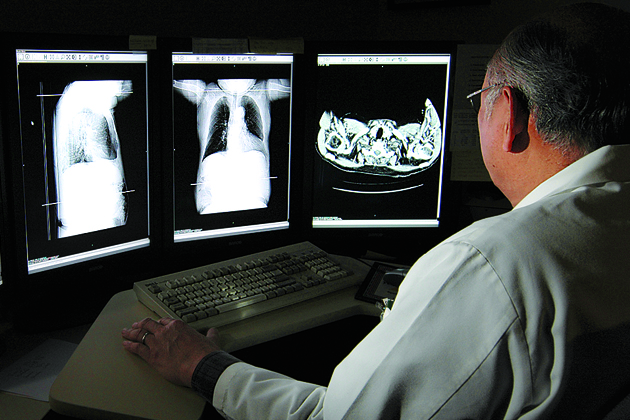
All of this may seem terribly basic, when businesses from Wal-Mart to the corner store went digital long ago. But for medicine, these technological upgrades have been revolutionary. Two decades ago, the Spokane Veterans Affairs Medical Center was, by VHA standards, a smallish facility, with 132 inpatient beds. But in terms of its operating protocols—and shortcomings—it was typical. Everything ran on paper, with charts, updated by hand, following patients from room to room. Handwritten prescriptions were passed to pharmacists, who counted pills and filled bottles. X-rays were developed on film and physically carried from laboratory to office, where they were analyzed on backlit screens. Nurses dispensed medication after a cursory check of the chart at the foot of a patient’s bed.
Today, patient records reside in a central server, accessible via laptop, and radiology images show up instantly on high-resolution computer screens. When a prescription is entered into a terminal and verified by a pharmacist, it goes to “the robot,” a glass-walled unit in the hospital pharmacy that sorts and packs the requested medication before sending it to a human pharmacist for inspection. And instead of fretting about giving a patient the wrong medication, nurses count on the system to watch their backs.
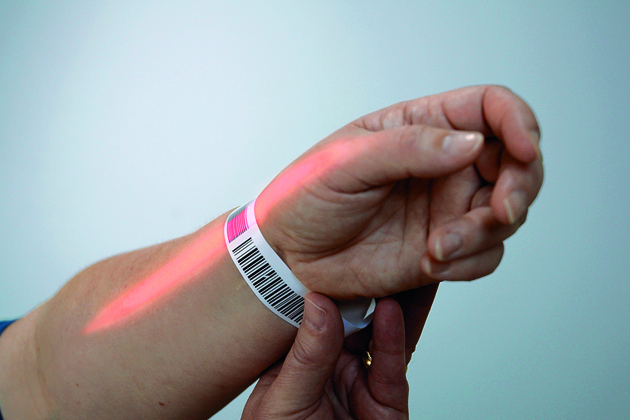
Eric Knievel, the Spokane hospital’s clinical applications coordinator, demonstrates by scanning a bar-coded patient bracelet into a wireless terminal on a cart. Then he scans the bar code on a medication vial. “The software checks to see whether it’s a valid order for that drug at that time in that dose by that method of administration,” Knievel says.
Spread across VHA facilities nationwide, these changes have transformed the hospital system from laggard to leader. In 2003 the New England Journal of Medicine judged the VHA’s system superior to fee-for-service Medicare on all 11 similar quality-of-care indicators from 1994 through 1999; in 2000 the VHA outperformed Medicare on 12 of 13 indicators. And in the 2003 State of Health Care Quality report published by the National Committee for Quality Assurance, the VHA reported scores that met or exceeded the ninetieth percentile for commercial plans in many categories.

DIGITIZATION SAVES MONEY AS WELL AS LIVES. After sinking more than $1 billion into its information system, the VHA reportedly spends an estimated $78 per patient per year to run it. That’s a fraction of the savings it achieves by reducing unnecessary tests and avoidable admissions. Proper pneumonia and influenza vaccinations alone save the VHA more than $100 per year for each patient who gets the shots. The result is a trend line not often seen in health care: falling per-patient expenditures.
Still, as sleek as the current VHA electronic health-record system is when compared with the U.S. health-care norm, “it’s a Model T compared with what we’ll have in the future,” says Robert Kolodner, the VHA’s acting chief health information officer. Illustrating the gap between what is and what should be, a recent study of a Salt Lake City VA medical center published in the Archives of Internal Medicine found that while the current system eliminates the risk of illegible handwriting and flags such simple issues as drug allergies, it doesn’t necessarily help a doctor decide whether a particular drug is the best choice or is being administered in the ideal dosage.
The VHA’s current decision-support capability “isn’t a substitute for a functioning brain,’ says Kizer. But the next iteration might help considerably if it develops as planned. Called HealtheVet, it’s an information technology system that provides guidance for health-care providers and is designed to be continuously upgraded with such new technologies as voice recognition and remote diagnostics.
Phase one of the project is building a better database. Today’s VHA information systems are local, not national, with patient data residing in 128 different servers. And though those servers contain 650 million documents, clashing formats and protocols are making it difficult for computers to “understand” information from these different places.
“When we built the system twenty-some years ago, each hospital created its own database with its own terminology,” says Kolodner. “One facility may call a test ‘sodium,’ another ‘serum sodium,’ and another something else.” Doctors are used to this variability, but it’s a problem for software designed to provide doctors with automated clinical decision support.
“At the local level, they’re cleaning up the data, domain by domain,” says Kolodner. When each hospital has standardized its allergy files, for example, the data will flow into a central repository. When all domains are cleaned and collected, the system will become hub-and-spoke, with transactional computing and decision-support analysis done regionally and storage done centrally. The data gleaned from the regional HealtheVet system will alert doctors when a patient’s dosage needs adjusting or prompt them when an equally effective generic is available.
Meanwhile, entering a patient’s information into a central database shifts the emphasis from facility to patient. Today a VHA patient’s data is on the hard drive of each hospital at which he was treated. If he shows up at the emergency room of a different facility, this information must be retrieved from the other hospitals and is available only as text-based reports and results. With a central database, all patient information will be available to any VA facility. Moreover, each patient can have his own VHA online account. “Patients will have the same kinds of decision support their doctors do, so when they come in they’ll know these are the five things their provider should be doing for them,” says Kolodner.
With HealtheVet, the VHA could take medicine across the next digital frontier, ushering in an era in which telemedicine (by which patients are monitored and diagnosed at home via the Internet), ever more sophisticated decision support and other high-tech capabilities combine to provide a quality of care that’s closer to Star Trek than to Marcus Welby, M.D. The benefits of this initiative should eventually become available to community hospitals and other financially strapped operations, much as the VHA now makes its electronic health record software available for a nominal fee.
But this quantum leap has to be funded, and that’s not assured. Citing an outside study that found HealtheVet to be risky and poorly planned, the House Committee on Veterans’ Affairs recommended withholding development funding in fiscal year 2006. Kolodner’s response is that something this multifaceted is bound to have speed bumps. “There are funding issues for all government programs,” he says. “But one way or another, we have to make HealtheVet happen.”
Dossier
Digital Medicine: Implications for Healthcare Leaders, by Jeff Goldsmith (Health Administration Press, 2003). A helpful overview.
“The Veterans Health Administration: Quality, Value, Accountability and Information as Transforming Strategies for Patient-Centered Care,” by Jonathan B. Perlin et al., The American Journal of Managed Care, November 2004. A detailed account of the VHA’s transformation, from several of its chief architects.
Stay on the frontiers of medicine