Published On July 23, 2012
LIVING IN THE UNITED STATES, IT’S NOT EASY TO THINK ABOUT MALARIA, which ceased being a real problem here more than half a century ago. Yet this ancient scourge, which is thought to have killed more people than any other single cause, still ravages parts of Africa, Asia and Latin America. Half of the world’s population lives in malarial zones, and some 210 million people harbor malaria every year. Malaria kills more than half a million children under the age of five each year, mostly in sub-Saharan Africa. Yet many experts now think that as complex and dangerous a disease as malaria is, the time may be at hand to put an end to it—even though failure could be disastrous.
A previous global campaign to eradicate malaria began with enthusiasm, hubris and elation in the 1950s. It ended a decade later in defeat and despair. So it was a shock when the philanthropists Melinda and Bill Gates announced at their charitable foundation’s Malaria Forum in October 2007 a brazen goal to dig out malaria’s roots everywhere on earth, even in the farthest reaches of sub-Saharan Africa (where the 1950s campaign did not aspire to go). Others at the forum were even more surprised when Margaret Chan, director general of the World Health Organization, pledged her support and dared everyone to join. “The research community was galvanized,” says Ed Ryan, director of tropical medicine at Massachusetts General Hospital. “How do you wipe a disease off the face of the earth?”
For smallpox, polio and most other infectious diseases, that question had a relatively simple answer. Because they’re caused by viruses and are passed from person to person, everyone within an infected person’s circle of interactions can be vaccinated or treated. When no more circles appear, the disease is gone forever. But malaria is different. It is a mosquito-borne illness caused by a parasite that cycles relentlessly between humans and the mosquitoes that frequent rainy seasons and tropical regions. You can’t draw circles around swarming mosquitoes, and just one parasite from one infected mosquito can generate billions of offspring within weeks—and if just one infected person transmits a parasite to one mosquito, that mosquito can infect many more people. What’s more, that’s only the beginning of the challenges of eradicating malaria.
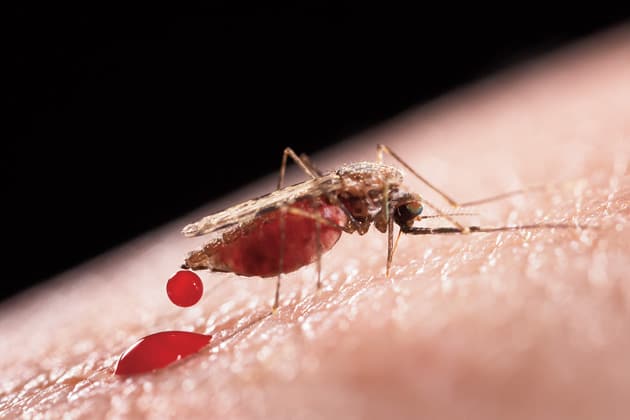
WHEN A MOSQUITO TRANSMITS PLASMODIUM PARASITES TO A HUMAN, other mosquitoes pick up the parasites when they bite that same victim. Infected mosquitoes carry tiny parasitic forms called sporozoites in their salivary glands, and when they bite, 100 or so sporozoites penetrate the skin and invade blood vessels, swimming to the liver. That initial transmission causes infection, but not yet disease, and this “pre-blood” stage is a bottleneck in the malarial life cycle when it might be possible for a drug or vaccine to kill the limited number of parasites that have been transmitted.
Within a week of invading liver cells, each sporozoite can give rise to tens of thousands of asexual merozoites. Each merozoite, in turn, rapidly replicates, forming a grapelike cluster that ruptures into the bloodstream in the “blood stage” of infection. Billions of merozoites sicken the victim by invading red blood cells and hiding from the immune system as they consume the heme molecule in hemoglobin, causing anemia and weakness. The sequestered parasite pushes proteins through the blood cell’s membrane. Those proteins are sticky and adhere to blood vessels in organs—especially in the brain, causing often—fatal cerebral malaria with coma, and in the placenta, endangering both mother and child.
Meanwhile, some merozoites develop into sexual gametocytes. Now begins the “mosquito stage” of the life cycle, another bottleneck available to therapeutic intervention. A mosquito biting the infected person will ingest a few gametocytes, and within two weeks those parasites will develop into sporozoites and travel to the salivary glands, ready for transmission to the next human.

PAUL HAHN/IAIF/REDUX PICTURES
THEORETICALLY, ELIMINATING ANY OF THE THREE LINKS IN THE DISEASE CHAIN—mosquito, parasite or human infection—could eradicate malaria. The most successful campaign, led by Fred Soper of the Rockefeller Foundation, focused on annihilating the mosquito. In the 1930s, African Anopheles gambiae, the species of mosquito that carries the deadliest form of parasite, Plasmodium falciparum, arrived in Brazil on a French ship. Soper pursued the African mosquito with military precision, draining breeding grounds and spraying afflicted areas with insecticides, and within two years he had eliminated the insects.
That triumph helped inspire the global campaign to eradicate malaria worldwide during the 1950s. By then, two scientific advances seemed ready to help break the chain of transmission: an easily tolerated antimalaria drug called chloroquine that cleared parasites from an infected person’s bloodstream, and the insecticide DDT. Public health officials swooped into remote villages, passing out chloroquine (even adding it to table salt) and spraying houses with DDT. But they largely bypassed sub-Saharan Africa, where transmission rates were so high that even in that age of optimism, breaking the chain seemed hopeless. In many places the work paid off, with the incidence of malaria falling dramatically. In Sri Lanka (then Ceylon), for example, cases fell from millions a year to 18 in 1963. Thirty-seven countries eliminated malaria entirely.
But in vast areas of the earth, malaria rebounded, for reasons that seem obvious in retrospect. “The harder you push, the more selective pressure you put on the mosquitoes and parasites to develop resistance, leaving people worse off than before,” says Jamie Maguire, senior physician in infectious diseases at Brigham and Women’s Hospital in Boston. Threatened by just one drug and a single insecticide, the parasite and mosquitoes evolved to defeat them and were soon flourishing again as DDT and chloroquine lost their effectiveness. Cases in Sri Lanka soared to an estimated 500,000 in 1969. In India the incidence doubled to 1 million.
People also succumbed to malaria at higher rates than before—not just because the drugs were ineffective but also because of lost immunity. Those who grow up where malaria is endemic are repeatedly bitten and infected, and when children survive malaria they acquire a limited, short-term immunity. It’s not total and lifelong, as in those who survive smallpox or measles, but the ongoing bites by infected mosquitoes serve as a kind of booster shot that keeps most adults from having much more than mild flu-like symptoms. Yet because the parasites remain in their systems, even infected people who don’t seem sick can transmit malaria to mosquitoes, which then infect neighbors, children and travelers who may not have the same level of immunity. And in locations that had eliminated malaria for a number of years, people again became completely vulnerable to a disease that has become harder to treat.
The eradication campaign was abandoned in 1969, and during the 1970s the notion of stopping transmission between mosquito and human was replaced by efforts simply to identify those who had malaria and try to keep them alive. Research also flagged—the campaign of the 1950s and ’60s had eradicated malariologists, it was said, not malaria, with few new scientists opting to train to fight a disease that had been thought to be on its way out. By 2000 more than 3 million people a year were still dying of malaria, WHO estimated.
SCIENCE PHOTO
EVEN DURING THOSE LOST DECADES, THE STAGE WAS QUIETLY BEING SET for today’s new push for eradication. Though neither sophisticated drugs nor a vaccine was in sight, research and funding for the fight against malaria were again on the upswing, the genomes of parasite and mosquito were being decoded, and the molecular machinery that allows parasites to evade the immune systems of both mosquitoes and humans was coming to light.
Meanwhile, low-tech tools had begun cutting deaths significantly. During the early 1990s, some countries switched from chloroquine to sulfadoxine-pyrimethamine, which probably reduced transmission before resistance soared a few years later. By the turn of the century, a highly effective new drug, artemisinin, derived from a Chinese wormwood plant, became available. To prevent or at least delay artemisinin resistance, it was combined with other drugs in a three-day treatment known as ACT—artemisinin combination therapy.
Then, during the 2000s, an orchestrated effort to distribute mosquito nets treated with insecticide also began paying off. The treated nets are a “brilliant intervention,” says Richard Steketee, science director of the malaria control program PATH, a global nonprofit based in Seattle. They protect people sleeping under them and kill mosquitoes that land on them, benefiting even those sleeping outside the nets. In pilot programs, mosquito net distribution was supplemented with residual indoor spraying of insecticides, an intervention tailored to the biology of the African mosquito,Anopheles gambiae. The insects come inside after dark, and even if they manage to bite someone, they’ll fly to a wall, heavy with blood—and soon die from the insecticide on the wall. Providing preventive drugs to pregnant women and infants, both especially vulnerable to malaria, also saved lives.
Numerous clinical studies, surveys and observations have since confirmed the value of a decade’s worth of mosquito nets, residual spraying and preventive interventions. Malaria deaths dropped from some 3 million annually in 2000 to between 655,000 and 1.2 million in 2010 (according, respectively, to a 2012 WHO report and a study published in The Lancet). But are nets and insecticide enough to get rid of malaria once and for all? Or do we still lack crucial resources—in particular, a vaccine? “While these low-tech tools will take us far, they’ll never go the last mile,” says Pedro Alonso, head of the Gates-funded Malaria Eradication Research Agenda (malERA), which is focused on finding the right combination of vaccines and new drugs to break the chain of transmission.
As game-changing as a vaccine would be—and as crucial as vaccines have been in fighting smallpox, polio and measles, among other diseases—the complexity of malaria poses obstacles that have often seemed insurmountable. Surviving a single exposure to the natural pathogens that cause those other diseases provides complete, lifelong immunity, which suggests an obvious path for developing a vaccine, but that doesn’t happen when someone gets malaria. A vaccine against that disease must do better than the natural infection in providing a more robust and long-lasting immunity—and it may never be able to provide permanent protection, says Christopher Plowe, who leads the malaria group in the Center for Vaccine Development at the University of Maryland School of Medicine.
The first vaccine to show meaningful clinical protection takes aim at the pre-blood stage that causes initial infection in humans. Known as RTS,S, it’s now being tested in almost 16,000 children and infants in seven African nations. RTS,S contains a malarial parasite protein (circumsporozoite protein, or CSP) that elicits an antibody response in human immune cells. According to preliminary results published in the Nov. 17, 2011 issue of The New England Journal of Medicine, the vaccine reduced clinical disease by about half and severe malaria by 35% a year after vaccination. That was much better than previous efforts, says Plowe, who was not involved in the trial. “But it’s still not nearly good enough for eradication.” Plowe also helped lead a small trial, with 400 children in Mali, of a blood stage vaccine containing a merozoite antigen that reduced the risk of malaria by just 20%. Even if researchers could create a better blood stage vaccine able to curb malaria in infected patients, it would be unlikely to wipe out the billions of merozoites that would by then be in a person’s bloodstream. So though it might reduce illness and death, people could remain asymptomatically infected—and could continue to transmit the parasite to mosquitoes and then to new human victims.
But scientists think a blood stage vaccine that benefits an infected person might be combined with vaccines being developed to target the second transmission choke point, when mosquitoes suck up the sexual gametocytes. Such a vaccine would be given to people to prevent the gametocytes from maturing once inside the mosquito. It wouldn’t directly protect the person receiving the therapy, but it would help the person’s family and community by reducing the number of infected mosquitoes in what has been dubbed a “do unto others” strategy.
Plowe is most excited about his collaboration on a whole parasite vaccine that puts a modern twist on an old idea—using live but weakened, or attenuated, organisms (in this case, an entire parasite) in vaccines. Attenuated pathogens can’t cause disease but do stimulate a protective immune response. In 2003, Steve Hoffman, former director of the malaria program at the Naval Medical Research Center, founded a company, Sanaria, to develop a new whole parasite vaccine. Sanaria researchers injected irradiated sporozoites into the skin of 80 healthy volunteers. In that trial, reported in the Oct. 28, 2011 issue of Science, the vaccine was safe and well tolerated, but not particularly effective. But the study also showed that injecting nonhuman primates with the same vaccine intravenously works much better than just injecting it into the skin. Intravenous injections wouldn’t be practical in delivering the vaccine to millions of people in developing nations, so the trick now is to make a single injection into the skin work as well as 1,000 mosquito bites. “That’s a bioengineering problem,” Plowe says. “It can be solved.”
HAVING BETTER DRUGS WOULD ALSO HELP IN THE ERADICATION EFFORT—and will be vital as resistance to artemisinin, already appearing in parts of Asia, becomes widespread. Artemisinin and other drugs intervene at the blood stage, but new drugs might block the transmission of parasites at the bottlenecks. While it has been difficult to grow malaria parasites in tissue cultures, an international research collaboration has devised laboratory assays for each life stage of the parasite, which it published in the Feb. 21, 2012 issue of PLoS Medicine.
Meanwhile, another possible approach to aid in eradication—breeding mosquitoes incapable of transmitting parasites—remains the focus of much of the research being funded by the National Institutes of Health. Yet even if researchers were to succeed, managing to replace all of the insects in malarial hot spots is likely to be problematic.
Whatever combination of tools and techniques is used in the effort to eliminate malaria, it’s likely to take a long time to succeed. Even the most ardent advocates of eradication don’t dare talk of a 10-year plan, as they did in the 1950s. “Theoretically there is no reason we can’t eradicate malaria,” says Brigham and Women’s Maguire. “Realistically, though, it will come down to political will, social programs and funding.”
Dossier
“Net Benefits: A Multicountry Analysis of Observational Data Examining Associations Between Insecticide-Treated Mosquito Nets and Health Outcomes,” by Stephen S. Lim et al., PLoS Medicine, Sept. 6, 2011. By analyzing observational data, these researchers confirm that routine use of insecticide-treated bed nets provides the reduction in malaria cases predicted by controlled clinical trials.
“Vaccines for Malaria: How Close Are We?” by Mahamadou A. Thera and Christopher V. Plowe, Annual Review of Medicine, February 2012. The authors conclude that a reinvention of an old idea—a vaccine that uses an entire parasite rather than just one or more surface proteins from the parasite—may be the most successful approach.
“Some Lessons for the Future From the Global Malaria Eradication Programme (1955-1969),” by Jose A. Najera, Matiana Gonzalez-Silva and Pedro L. Alonso, PLoS Medicine, Jan. 25, 2011. The authors call for an end to today’s alternation between overly optimistic expectations and a “fire-fighting strategy” of selectively targeting areas that ends in “disappointment and abandonment.”
Stay on the frontiers of medicine
Related Stories
- Smoking Out Malaria
Almost eradicating the disease, as happened in the 1950s, led to a disastrous resurgence. Is now the time for a smarter, final push?
- Nature Bites Back
More than half of infectious diseases pass through animals first. A strain on their natural habitats may be making these ailments more dangerous.
- Dr. Exotica
Tending to recent immigrants and other travelers, Carlos Franco-Paredes diagnoses diseases that few other physicians in North America have ever seen.